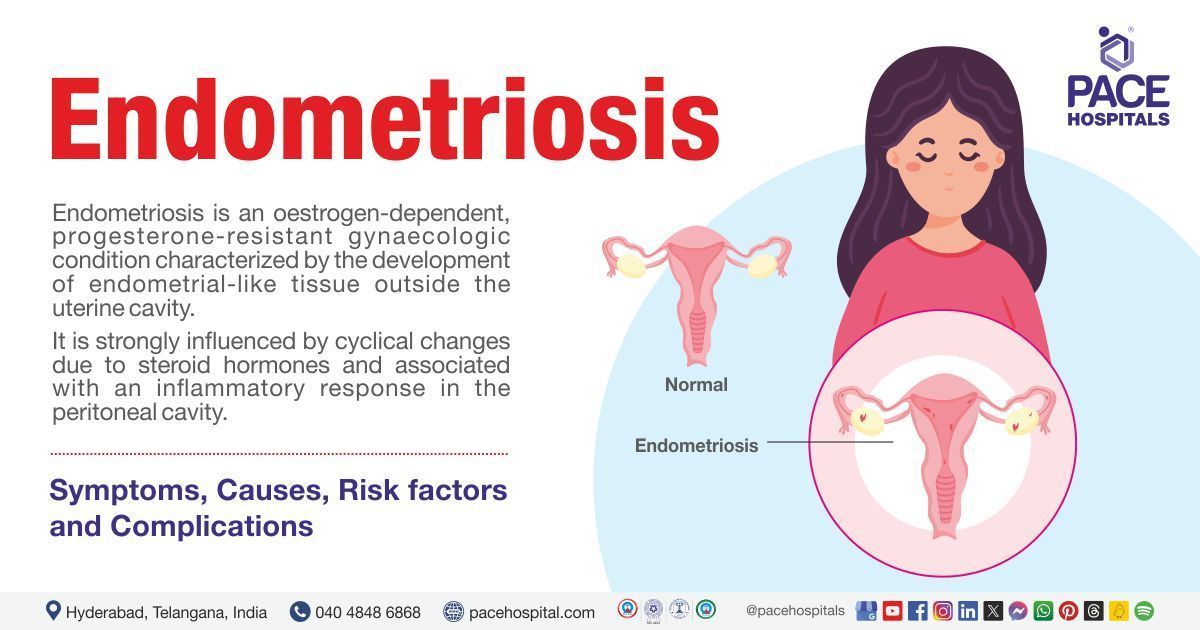
Best Hospital for Endometriosis Treatment in Hyderabad, India
At PACE Hospitals, we are dedicated to providing the best endometriosis treatment in Hyderabad, Telangana, India. Our advanced facilities are equipped with cutting-edge diagnostic technology, including high-resolution imaging, laparoscopic, and robotic-assisted procedures, ensuring precise evaluation of endometriosis severity. We provide a comprehensive range of treatment options, from medical management for pain relief to minimally invasive surgery for endometrial implant removal.
Our team of expert gynecologists and laparoscopic surgeons employs the latest surgical techniques, such as minimally invasive laparoscopy, to effectively alleviate pain and enhance fertility. Recognizing the complexities of endometriosis, we tailor personalized treatment plans to prioritize your comfort, recovery, and long-term health. With a patient-centric approach, we ensure clear communication, compassionate support, and active involvement in your treatment decisions every step of the way.
Book an appointment for Endometriosis Treatment
Endometriosis treatment appointment
Why Choose PACE Hospitals for Endometriosis Treatment?

Advanced Robotic-Assisted Laparoscopic Endometriosis Surgery
Best Gynecologists & Laparoscopic Surgeons in Hyderabad, India
24/7 Emergency Endometriosis Care & Advanced Pain Management
Affordable & Reliable Minimally Invasive Endometriosis Treatment
Comprehensive Endometriosis Evaluation: Diagnosis & Treatment Planning
The endometriosis evaluation may depend on factors such as history and physical examination, which help the gynaecologist confirm the diagnosis. Endometriosis is subject to the treatment of painful symptoms.
The gynaecologist considers the following before selecting the appropriate tests to diagnose endometriosis.
- The presented signs and symptoms
- Age, family history, and general health of the suspected patient
- Medical history and medication history
- The results of previous medical tests
The presented signs and symptoms: The diagnosis of endometriosis might be considered in females (aged 17 and under) presenting with one or more of the symptoms such as chronic pelvic pain, dysmenorrhea (heavy menstrual bleeding), deep dyspareunia (painful intercourse), cyclical gastrointestinal (dyschezia: difficulty pooping or painful defecation) and urinary symptoms (hematuria: blood in urine or dysuria: painful urination) or infertility in association with one or more of the preceding signs or symptoms.
Suppose the patient has endometriosis at extra-abdominal sites. In that case, they may present with shoulder tip pain, cyclical cough or haemoptysis (coughing of blood) or chest pain, and catamenial pneumothorax (spontaneous and recurrent pneumothorax occurring within 72 hours before or after the onset of menstruation).
Endometriosis may not be definitively diagnosed by symptoms alone. A gynaecologist may suspect this condition if the patient has the above-mentioned symptoms. However, it can also be suspected if the patient is present with a persistent ovarian cyst.
Age, family history, and general health of the suspected patient: A gynaecologist considers the age and family history of the patient to estimate the risk of endometriosis and wants to know about the regularity of menstrual periods and the length of menstrual cycle and overall health condition to choose proper diagnosis and treatment.
Medical history and medication history: A gynaecologist asks detailed questions about the medical history when evaluating a woman for endometriosis to recognize co-exiting gynaecological conditions and their association with endometriosis. They also assess signs and symptoms that mimic endometriosis.
The woman's hormonal status plays a vital role in endometriosis; therefore, a gynaecologist may ask the patient questions about the use of any previous hormonal treatments.
A gynaecologist may want to know the medication history of the patient (e.g., fertility drugs or contraceptives) to determine whether these drugs are interfering with treatment options.
The results of previous medical tests: A gynaecologist may ask about the reports of earlier medical tests to get valuable information to confirm the presence of endometriosis in a patient and to choose the proper diagnosis and treatment.
Endometriosis diagnosis
The diagnosis of endometriosis is initially made based on the patient's medical history, signs, and symptoms, then confirmed by physical examination and imaging methods. Finally, a histological examination of specimens collected during laparoscopy provides confirmation, such as:
Physical examination
- Pelvic examination
Imaging tests
- Ultrasound
- Transvaginal ultrasound
Biomarkers
- Serum CA-125
Minimally invasive techniques
- Diagnostic laparoscopy
Physical examination
Gynaecologists may suspect endometriosis if they notice specific findings of a pelvic exam, such as abdominal masses (lumps in the abdomen) and pelvic signs, including reduced organ mobility and enlargement, tender nodularity, and visible vaginal endometriotic lesions.
During a combined rectal and vaginal exam, a tender nodule may be felt by the gynaecologists near the cervix, or the uterus may lack mobility (may not move freely) because of scar tissue and adhesions (fibrous bands of tissue binding organs together). There will be an enlarged one or both ovaries or fixed in position. However, rarely implants of endometriosis may be visible in the vagina or cervix.
However, vaginal examination is not appropriate in women who have not had previous sexual intercourse, but rectal examination can be helpful for diagnosis.
Imaging tests
Transvaginal sonography (TVS): Transvaginal sonography (TVS) can be used to diagnose rectal endometriosis in cases with suspected deep infiltrating endometriosis (found deep within the tissue or organ). It can be used to diagnose an adnexal mass (mass in the ovary, fallopian tube, or surrounding connective tissues) suspected of endometriosis to diagnose ovarian endometriosis.
Magnetic resonance imaging (MRI): Pelvic MRI can be used to assess the extent of deep endometriosis involving the bladder, bowel, or ureter. However, pelvic MRI may not be considered to be as the primary investigation for diagnosing endometriosis in women with signs or symptoms suggestive of endometriosis, and it is not helpful to diagnose or exclude peritoneal endometriosis. MRI test is recommended when ultrasound (USG) examination is inconclusive or when there is deep infiltrating endometriosis, and the patient requires extensive surgery to rule out malignancy as it may characterize the lesion.
Biomarkers
Serum cancer antigen (CA-125) has been used as a glycoprotein biomarker that is usually performed in women has pelvic masses (abnormal growths in the pelvic area) such as endometriosis, and it is also helpful in evaluating patients suspected of having endometriosis.
As per the studies, it was found that endometriosis may raise the risk of ovarian cancer. Hence, gynaecologists may prefer this test to monitor ovarian cancer therapy and recurrences because CA - -125 serves as an ovarian cancer biomarker.
Serum CA-125 is also used to follow up on the recurrence of the endometriosis condition in patients with advanced endometriosis.
A study published in 1998 demonstrated that elevated CA-125 (>35 U/ml) was reported in 86.70% of women who have advanced endometriosis, while it is only 26.8% in patients suffering from minimal and mild endometriosis.
It was also observed that one year after therapy in women having previously had elevated levels of CA-125, the recurrence of endometriosis was not seen, CA-125 levels returned to normal.
However, CA-125 is not a specific biomarker for endometriosis and may not be recommended for routine clinical use. In some cases, it may be of value for treatment follow-up.
Minimally invasive techniques
Diagnostic laparoscopy: The gold standard for diagnosing endometriosis includes the combination of laparoscopy and the histological verification of endometrial glands or stroma.
Usually, laparoscopy suggests if the patient is present with signs of deep endometriosis or ovarian endometriosis that are found on physical examination and imaging, especially in adolescents and young adults.
This method might be used in combination with histopathology for diagnosing endometriosis. For this procedure, the patient will be given a general anaesthetic (put to sleep), and a laparoscope (special viewing tube) with a light on the end will be passed into the patient's body. The laparoscope has a tiny camera transmits images to a video monitor, so the gynaecologist can view the endometriosis tissue.
The gynaecologist may take a biopsy (small tissue sample) for laboratory testing or insert other surgical instruments to treat the endometriosis.
The location of the body where the laparoscope is inserted depends on where the gynaecologist suspects the endometriosis tissue to be; because many patients have symptoms around their pelvis and lower abdomen.
Endometriosis stages
The staging system of endometriosis was divided into four stages:
| Stages of endometriosis | Revised American Society for Reproductive Medicine (rASRM) classification (scoring system) | Intensity of condition | Compromises |
|---|---|---|---|
| Stage I | 1-5 points | Minimal | Few superficial endometriotic spots or adhesions |
| Stage II | 6-15 points | Mild | Few, deep peritoneal lesions alone or in combination with superficial lesions and filmy adhesions |
| Stage III | 16-40 points | Moderate | Endometrioma by itself or in combination with superficial or deep endometriosis and dense adhesions |
| Stage IV | > 40 points | Severe | Bilateral ovarian endometrioma or dense adhesions leading to a partial or complete obliteration of the pelvis. |
✅Endometriosis differential diagnosis
A differential diagnosis is a list of possible medical conditions or diseases that can share the same symptoms as endometriosis in a woman. Endometriosis has an extensive differential diagnosis that includes the following.
Chronic pelvic pain
Irritable bowel syndrome: Altered bowel habits with abdominal pain or bloating
Pelvic inflammatory disease: Abnormal vaginal discharge, fever, irregular bleeding
Pelvic adhesions (bands of scar-like tissue): Ovulatory pain, history of pelvic inflammatory disease, or extensive abdominal surgeries
Painful bladder syndrome: Urinary symptoms (urgency, frequency, nocturia) with routine urinalysis, pain in the bladder based on vaginal exam
Myofascial pain (a chronic condition that affects the muscles and the fascia (thin connective tissue) around them): Constant pain that worsens with activity, tender pelvic floor muscles
Pelvic venous disorders (a condition where the normal valves in pelvic veins do not work properly, leading to pelvic vein enlargement and pain): Pelvic heaviness, worse with standing, better supine, postcoital ache.
Dysmenorrhea (pain during the menstrual cycle)
Primary dysmenorrhea (recurrent pain with no identifiable cause): Short-lasting (< 72 h), responsive to nonsteroidal anti-inflammatory drugs Adenomyosis Heavy menstrual bleeding, boggy tender uterus Uterine fibroids Heavy or intermenstrual bleeding, pressure symptoms, bulky uterus Cervical stenosis Decreased flow or amenorrhea, history of surgery on cervix Obstructive lesions of the genital tract amenorrhea with cyclical pain, visible bulge at introitus>72 h), responsive to nonsteroidal anti-inflammatory drugs).
Adenomyosis (growth of endometrial tissue into the muscular wall of the uterus): Adenomyosis Heavy menstrual bleeding, boggy, tender uterus.
Uterine fibroids (muscular tumors that grow in the wall of the uterus): Heavy or intermenstrual bleeding, pressure symptoms, bulky uterus.
Cervical stenosis (cervix of the female reproductive system is either too narrow or completely closed): Decreased flow or amenorrhea, history of surgery on cervix.
Obstructive lesions of the genital tract: Amenorrhea with cyclical pain, visible bulge at introitus (opening of the vagina, which leads to the vaginal canal).
Deep dyspareunia (painful intercourse)
Pelvic masses (abnormal growths): Pelvic pressure, enlarged uterus or adnexae.
Cervicitis (irritation or infection of the cervix): Abnormal discharge, postcoital spotting, localized tenderness to palpation, erythema of cervix.
Painful bladder syndrome (Interstitial cystitis (IC), often called painful bladder syndrome, causes long-term pain or discomfort in the bladder and abdominal area): Urinary symptoms (urgency, frequency, nocturia) with normal urinalysis, pain at bladder based on vaginal exam.
✅Considerations of a gynaecologist before treatment
A gynaecologist considers the following before planning treatment:
- Patient age
- Whether the patient is having pain or infertility
- Whether the patient wants to become pregnant
- Whether the patient has tried any of the treatments before
Treatment may not be required if the patient's symptoms are mild and there are no fertility issues. In approximately 1/3rd of cases, endometriosis gets better by itself without any treatment.
Endometriosis treatment
The management of endometriosis in a suspected patient may depend on the patient's age, the degree of pain and other symptoms, desire for fertility, high-risk co-morbidities, the impact on their capacity to work, and their quality of life.
Treatment options for endometriosis for patients who are suffering from symptomatic endometriosis are hormonal therapies to suppress the menstruation and ovulation process, surgical treatment, or a combination of both treatments.
Medical management of endometriosis
- Hormonal treatments
- Single hormonal treatments
- Combined hormonal treatment
- Other hormonal treatment options
- Pain medications
Surgical management of endometriosis
- Conservative surgery
- Endometriosis laparoscopic surgery
- Radical surgery
Medical management of endometriosis
The goal of medical management is to control the patient's symptoms and includes both hormonal and non-hormonal treatments.
Hormonal treatment can be given to do the hormonal suppression of endometriotic lesions and is especially effective when amenorrhea (absence of menstruation) occurs via down-regulation of the hypothalamic-pituitary-ovarian axis (mainly responsible for regulating menstrual cycle).
However, hormonal treatment may not stop disease progression, and there are patients for whom specific hormonal treatments will not be appropriate, for instance, A recent or current history of breast cancer or a history of liver tumors.
It is estimated that approximately 50 in 100 women may have a recurrence of endometriosis symptoms within five years if medical treatment is stopped.
A step-wise medical treatment strategy: The first line of treatment for women with endometriosis who do not wish to become pregnant in the near future is hormonal medications and analgesics if required.
- Hormonal treatments: Hormonal treatments aim to stop the production of oestrogen hormone in the patient's body. This is because oestrogen leads to the growth and shedding of endometriosis. The endometriosis tissue can be reduced without exposure to oestrogen, which helps to ease the symptoms of this condition. However, hormone treatments do not affect adhesions ('sticky' areas of endometriosis), which can cause organs to fuse together and cannot improve fertility. These treatments aim to suppress ovulation if that process is painful and the menstrual cycle to create amenorrhea. Hormonal treatments are contraceptives and, therefore, are not appropriate for women who are trying to get pregnant, those who experience adverse effects with hormonal medicines, have contraindications to their use, or do not wish to use them.
- Single hormonal treatments: Usually, a three- to six-month (3-6) therapeutic trial with hormonal treatment will be used to manage the signs and symptoms of the patient and help strengthen a clinical diagnosis. Some hormones will be given in high-dose to treat endometriosis and its related pelvic pain, where it suppresses the hypothalamic-pituitary-ovarian axis to inhibit the ovulation process and reduce circulating oestrogen levels. This treatment also has a direct, additional effect on the endometrium, causing the atrophic change to both endometriotic lesions and endometrium.
- Combined hormonal treatment: Combined hormonal treatment is an alternative first-line treatment if single hormonal treatments are unsuitable or not tolerated by patients.
- Other hormonal treatment options: Other hormonal treatment options are used to bring temporary menopause by reducing the production of oestrogen for endometriosis patients. Gynaecologists sometimes give these drugs to patients before surgery to help decrease the amount of endometrial tissue. They're also offered as a form of long-term medical management. The injections are given either every 4 or 12 weeks.
- Pain medications: Non-steroidal anti-inflammatory drugs (NSAIDs) are the preferred treatment for endometriosis pain management. They act against inflammation and relieve pain and discomfort.
Surgical management of endometriosis
Surgical treatment is effective for reducing symptoms such as pain and may increase fertility in patients with reduced fertility.
In women with endometriosis-related pain, surgery is indicated in the following cases:
- If the woman does not wish to or cannot take the medical therapies
- Patients seeking fertility with pain
- Patients with deep endometriosis
- During concomitant management of other gynaecologic conditions
In women with endometriosis-related subfertility (a failure to become pregnant after one year of unprotected regular sexual intercourse), surgery may be indicated in:
- When a patient requests surgery as an alternative to assisted reproductive technology (ART)
- Women with hydrosalpinges undergoing IVF
- Management of ovarian endometriomas in specific circumstances
Even with surgery, there is no guarantee of complete eradication as it may recur because recurrence rates for endometriosis are often high and may require further surgery.20–40% of women may re-develop symptoms within five years of surgery. However, surgery, along with hormonal treatments, may reduce the risk of recurrence and the need for further surgery.
However, the success rate of surgical treatment of endometriosis depends on the age of the patient (because the effectiveness of surgery is higher in older women because of the natural decline in oestrogen production), the type of symptoms, the severity of the condition and its location.
Surgery for endometriosis is divided into two strategies:
- Conservative surgery
- Radical surgery
- Conservative surgery (or surgery with preservation of fertility): This surgery often involves laparoscopy to remove visible endometriosis lesions and preserve pelvic anatomy. It is the more common surgical approach, which is helpful in significantly reducing pain in the majority of patients and, in some cases, improving fertility. However, the rate of symptom recurrence is higher than with more non-preservative methods.
- Endometriosis laparoscopic surgery: During a laparoscopy, tissue of the endometriosis can be destroyed or cut out using minor cuts with tiny instruments that are inserted into the body. Laparoscopy is used to diagnose (detect) and treat endometriosis. All stages of endometriosis can be successfully treated with this technique. A laser, heat, or an electric current may be applied to destroy the tissue patches. Although this kind of surgery can relieve the patient's symptoms, they may sometimes reoccur, especially if some tissue of endometriosis is left behind at the time of surgery.
- Radical surgery: It is the surgery that is limited for a woman suffering from endometriosis who does not wish to conceive, and other treatments haven't been successful in them. It is indicated chiefly for symptoms of pain that fail to respond to conservative treatment. Procedures (aggressive options) include hysterectomy, oophorectomy, salpingo-oophorectomy, appendicectomy, and the cutting off of deeply infiltrating endometriosis, possibly involving bowel resection. The standard treatment of endometriosis in women who have a suitable number of babies is surgery, including hysterectomy and bilateral salpingo-oophorectomy. Removing all visible peritoneal lesions along with the uterus is the gold standard. Whereas laparotomy (open surgery) has been the open (traditional) approach for most of these procedures, modern alternatives such as vaginal and laparoscopic surgery will be used for many of these cases. Preoperative (before surgery) and postoperative (after surgery) medical therapy has a limited role in these surgeries, whereas postoperative hormone replacement therapy after bilateral oophorectomy is generally recommended. Women undergoing radical surgery should be counselled about the possibility of endometriosis symptoms persisting even after
hysterectomy and complete bilateral oophorectomy and the adverse effects associated with early, medically induced menopause.
Endometriosis Surgery Cost in Hyderabad, India
Endometriosis surgery cost in Hyderabad, India ranges varies from ₹70,000 to ₹1,15,000 (US$876 to US$1,342). However, the actual cost of endometriosis surgery may vary depending on several factors such as:
- Type of Surgery – Laparoscopic, laparotomy, or hysterectomy
- Patient Age & Severity of Condition – The complexity of the case and the patient's overall health
- Hospital Stay & Facilities – Length of hospital stay and the type of room/facilities chosen
- Pre-operative Assessments – Blood tests, imaging studies, and other diagnostic evaluations
- Expertise of Specialists – Experience and credentials of gynecologists and laparoscopic surgeons
- Health Insurance Coverage – Availability of cashless treatment or corporate medical approvals
Cost of Laparoscopic Endometriosis Surgery in Hyderabad, India
Laparoscopic endometriosis surgery cost in Hyderabad, India varies from ₹1,20,000 to ₹1,45,000 (US$1,402 to US$1,694). At PACE Hospitals, we strive to provide transparent and affordable pricing while maintaining the highest standards of medical care. The cost of endometriosis surgery can vary depending on several factors, including the type of surgery, the complexity of the case, and the specific treatment plan tailored to your needs. We are committed to offering comprehensive care and ensuring you receive the best possible treatment without financial burden.
Frequently Asked Questions (FAQs) on Endometriosis treatment
What is the link between infertility and endometriosis?
Infertility is one of the most common symptoms of endometriosis. Approximately 4% of women with infertility have endometriosis. Endometriosis causes inflammation and may damage the sperm or egg or interfere with movement through the fallopian tubes and womb (uterus). The fallopian tubes may be blocked by scar tissue or adhesions in severe cases of endometriosis.
How does endometriosis cause problems?
Endometriosis is an oestrogen-dependent and progesterone-resistant gynaecologic condition where the endometriosis tissue responds to changes in a hormone, especially oestrogen. Endometriosis tissue may grow and shed as the uterine lining does during every menstrual cycle.
This tissue causes inflammation, irritation, and swelling around the surrounding tissues, leading to fibrosis (scar formation) and adhesion development, which in turn contributes to the development of symptoms and physical distortion of pelvic anatomy (changes in the normal shape, structure, and positioning of organs.
Is endometriosis the same as endometrial cancer?
No, endometriosis is not the same as endometrial cancer; both are different conditions. Endometrial cancer develops in the endometrium (lining of the inside of the uterus), where the cells in the endometrium start to grow out of control. Endometriosis is an oestrogen-dependent condition in which endometrium-like tissue grows outside the uterus.
Where does endometriosis occur?
Endometrial tissue (often called implants) is mainly found in the following places:
- Peritoneum
- Ovaries
- Fallopian tubes
- Cul-de-sac (the space behind the uterus)
- Outer surfaces of the uterus, bladder, ureters, intestines, and rectum
Other sites for growth may include vagina, vulva, cervix, bowel, bladder or rectum. Rarely, endometriosis may appear in other parts, such as lungs, brain, skin.
What if I still have severe pain that does not go away even after I have had treatment?
Hysterectomy may be considered a "last resort" option if the patient is having severe pain and that does not go away after treatment. Endometriosis is less likely to cause pain in the future if the patient's ovaries are removed at the time of hysterectomy. However, surgical treatment aims to remove as much as possible of the endometriosis tissue that is found outside the uterus.
Does endometriosis ever go away on its own?
In some women diagnosed with endometriosis, endometriosis patches go away on their own in some woman diagnosed with endometriosis. Treatment may not be required if the patient's symptoms are mild and there are no fertility issues. In approximately 1/3rd of cases, endometriosis gets better by itself without any treatment.
After menopause, most women may see fewer symptoms of endometriosis because there is a drop in hormones such as oestrogen, and the growths of endometriosis gradually shrink. However, this does not happen in all women. If a woman takes hormonal treatments for symptoms of menopause, there is a chance of returning the pain symptoms and growth.